It’s cold and uncomfortable and leads to extra hours of inconvenience, but women could lose less hair during chemotherapy if a trial at Orange hospital is successful.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
The oncology unit is trialling cold cap technology among three breast cancer patients who require three months of a chemotherapy, which generally causes hair loss, so results can be gauged in a fairly quick time frame.
The cap keeps a patient’s scalp cool while they receive chemotherapy, reducing the blood flow to hair follicles.
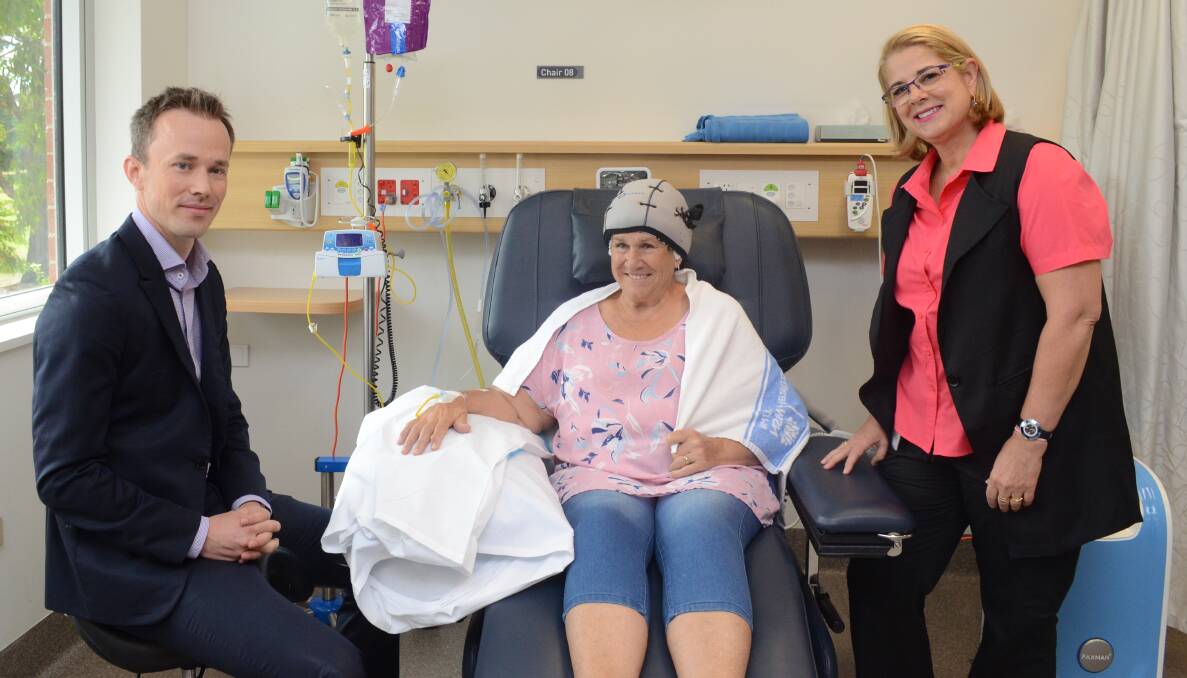
Medical oncologist Dr Peter Fox said it is the only technology of its kind in the Central West but because it adds two hours to usual chemotherapy, not all patients request it.
He said in Sydney they found between 10 per cent and 20 per cent of patients can’t stand the discomfort and because of the extra resources and time required, it was mostly private hospitals offering the treatment.
Until now, he said the closest hospital offering the treatment was in Campbelltown but unlike the US where patients would have to pay an extra $5000 on top of their treatment, in Australia it is free.
Dr Fox said cold caps started in the 1980s but began with ice bags taken out of a fridge and bandaged to a patient’s head.
He said those early treatments were not particularly successful but in the last 10 years more successful methods have been created.
Dr Fox said if the trial is successful and the hospital purchases the equipment it could mean woman from country towns could have the anonymity of walking down the street without people knowing they are going through chemotherapy or have cancer.
VIDEO: Ellen Davies of Portland discusses wearing a cold cap to reduce hair loss
Central West Cancer Service McGrath breast care nurse Sue Kuter said if the trial was successful, the unit would look at purchasing one of the $42,000 machines permanently for the hospital, and another could be bought for Bathurst.
As a result women in Parkes, Cowra, Lithgow, Forbes and Grenfell could receive the treatment and depending on the type of cancer and the chemotherapy required to treat it, some men could receive the treatment as well.
“Many women with a diagnosis of breast cancer actually fear alopecia and hair loss more than the chemotherapy treatment so it’s exciting to be able to offer them this opportunity,” Mrs Kuter said.
“The scalp cools the head down to under 22 degrees by running fluid through the cap which has been chilled to between -1 degrees and -5 degrees. This cools the blood flow to the hair follicles so they aren’t damaged.”
Mrs Kuter and Dr Fox tried the cold cap and said it was uncomfortable but eventually the head goes numb.
Dr Fox tried it for half an hour and said it was ducking his head in a pool of ice.
Patient, Ellen Davies from Portland, has had two treatments with the pilot treatment testing hair loss after four cycles of chemotherapy.
“When I was offered the cooling cap and to be part of the trial I was very happy to give it a go because I want to help provide results so it might be available for other women in the future,” Mrs Davies said.
“It’s a strange feeling having your head cooled down when the rest of your body remains at a normal temperature.
“My treatment goes for about six hours and I haven’t found it too taxing to use.”


